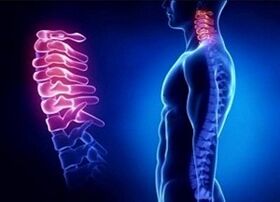
The 2nd degree osteochondrosis of the cervical region of the supporting pillar is a pathology that people of different eras face.Many ignore the symptoms of the initial phase of the disease, degenerative and dystrophic processes continue more actively, pain occurs.
Doctors advise paying attention to signs of osteochondrosis in the cervical area.Do not wait until the cartilage is destroyed between the discs, which will condemn the patient to constant pain, disorder of neck mobility.It is important to know: with a severe degree of discogenic pathology, brain hypoxia develops, dangerous cerebral disorders appear, and the risk of ischemic stroke increases.
General information
The first rate of the disease continues almost asymptomatic: sometimes poor neck pain occurs, with palpation you can feel a slight muscle tension.If you start timely treatment: gymnastics, taking analgesics, chondroprotectors, vitamins, massage, then it is only enough to stop the initial degeneration process.
In the absence of adequate treatment, the disease progresses.The second degree of osteochondrosis of the cervix of the spine is often detected by doctors in patients with complaints of headaches, unpleasant sensations when slopes and curves of the head, restriction of movements, tension of the neck and shoulder muscles.
Important points in 2 degrees of osteochondrosis in the cervical region:
- A fibrous ring cracks appear, the instability of the cervical spine develops;
- Criminations in the process of diffusion, which provides full nutrition of intervertebral discs, adversely affect the state of the cartilage tissue, the destruction of an important element begins.Violation of the depreciation setting structure leads to a decrease in the height of the disc, the beads approach each other, the movements of the head and neck cause pain;
- The pressure on the nerve roots increases, periodic pains appear.They can be eliminated with analgesics, but unpleasant sensations return soon after the drug expiration;
- In the second stage of the disease, there is no active compression of the vertebral artery, but patients feel other signs of pathology: lethargy, sleep disturbances, increased fatigue, decrease in performance levels;
- With cervical osteochondrosis, the pain is located not only in the problem area, but also spreads to the back of the head, the upper back, shoulders.Progression of the disease against the background of impaired intrigue of adjacent departments causes cerebral complications;
- In the absence of treatment, while maintaining the action of negative factors, the pathology goes to 3 degrees with active damage to the fibrous ring and the laying of the hyalin.Investigation is extension and intervertebral hernia, persistent pain during rubbing of vertebrae, problems with cervical area mobility and glossy exposed neurological disorders.
The reasons for developing pathology
Osteochondrosis in the cervical region develops against the backdrop of the following factors:
- hypothermia;
- violation of residence;
- Lack of calcium and vitamins;
- the landing habit, hanging, bending the lower head;
- long work on the computer;
- genetic predisposition;
- Cervical injuries;
- Excess load on the neck area, extremely active head movement;
- improper mineral metabolism for the origin of different pathologies;
- endocrine diseases;
- In the process of performing professional tasks, the head is often thrown again.
Osteochondrosis of the 2nd degree of cervical department code according to ICD - 10 m42.
Symptoms of cervical osteochondrosis
The progression of neck osteochondrosis indicates an increase in pain syndrome, an exacerbation in sensations of well -being, unpleasant in the upper back, especially after stress or prolonged stay in one position.The closer to each other's beads move, the more actively belong to the ligaments, the muscle strain seems to maintain the optimal position of the supporting pole.
Vertebrat subluxation in combination with a decrease in the impact of the muscle frame increases the discomfort in the affected area.The displacement of an elastic layer provokes increased pain during the return, bending and extension of the neck.
The disk extension changes the exact position of the neighboring bone structures, a violation of behavior appears.If you do not start treatment, continue the uncontrolled taking of sedatives, then you may soon encounter negative symptoms of 3 degrees of cervical osteochondrosis.
Troubleshooting
Treatment is performed by a vertebologist.You can also contact a neurologist.
To make a diagnosis, the profile specialist clarifies the clinical appearance and an anamnesis, describes an X -Ray of the cervical and MRI department.With severe muscle spasm, electromography is needed, if the patient complains of pronounced cerebral disorders, then shipping dopplerography will be needed.
Exactly!After diagnosis, doctors often notice that the patient develops a third degree of the disease, but the active progress of the process can still be recognized using instrumental studies.If you do not urgently begin treatment, then the symptoms of compression of the vertebral artery, followed by impaired cerebral circulation, the development of the hypoxia of an important organ, will soon appear in full strength.
The effective areas of therapy
After diagnosis, the doctor recommends eliminating the factors against which the disease progresses.If it stops degenerately - the dystrophic changes in the cartilage, then soon the pathological process will affect bone structures and blood vessels, a set of negative features will appear.With a severe degree of pathology, it is difficult to stop the process of cartilage destruction, damage to the fibrous ring, doctors detect the elongation and hernia of the disc.
medicaments
The doctor chooses several drug groups:
- Chondroprotectors.The compounds stop the destruction of the hyalin gasket, activate the process of regeneration of cartilage tissue.The course is from 3 months.
- NSAID.Eliminate inflammation in the nerve roots, reduce pain and swelling, improve the movement of the problem area.Drug Forms: Transdermal plaster, capsules, suspensions, tablets, gel, ointments.
- Musorexant.They help with painful muscle spasm, facilitate movement, relax muscle fibers.
- B vitamins.Neurotropic substances are essential for restoring the transmission of nerve impulses when they drank sensitive structures against the background of the progression of osteochondrosis.
- Analgesic.With headaches, discomfort against the backdrop of muscle tension, damage to the intervertebral discs, ordinary analgesics should be obtained.It is necessary to remember: soothing sedatives reduce discomfort, but without the treatment of osteochondrosis, unpleasant sensations in the cervical area, shoulders, headaches, cerebral disorders will intensify as orthopedic pathology progresses.
- Sedatives.Sleep urban disorder, headache, discomfort in head movements adversely affect the state of the nervous system.Patients become irritating, insomnia occurs more often.Herbal compounds and synthetic medicines help: desert tincture, soothing phytosbor, valerian in tablets and solution based on roots, mint boiling, lemon balm.
Corticosteroids and blockage of spine medication in 2 degrees of discogenic pathology in most cases are not needed: dystrophic and degenerative processes in intervertebral discs, adjacent tissue are not active enough to provoke painful pain.To relieve the condition of the complex of these medicines.It is impossible to use powerful analgesics without prescribing a doctor: with 2 degrees of illness, there is sufficient preparation of moderate exposure effects.
Other methods of treatment
The patient should remember: exclusively with medication it is impossible to stop the progression of cervical osteochondrosis.Complex therapy is a prerequisite for restoring the damping structure, reduction of pain, elimination of muscle spasms and normalization of neck mobility.
Effective methods:
- Neck massage, including point;
- the use of Lyapko and the many more complete Kuznetsov;
- Hirudotherapy;
- acupuncture;
- Physiotherapy: Ozokerite applications, Mudlet, UHF, Electrical and Phonorophoresis with effective analgesic and anti-inflammatory drugs;
- physiotherapy exercises and special exercises for cervical osteochondrosis;
- manual therapy;
- Wearing a shants collar.
Potential complications
Without time, complex, osteochondrosis progresses, brain dysfunctions appear against the backdrop of vertebral artery compression, backed nerve roots.The longer the patient removes the visit to a neurologist or a vertebologist, the more active the intervertebral discs are destroyed, the risk of severe cerebral disorders increases.
The progression of cervical osteochondrosis often provokes various pathologies and dangerous conditions:
- dizziness for cervical osteochondrosis in combination with nausea and pallor;
- ischemic stroke;
- Scoliotic changes;
- The development of a low neck -oriented cone, which is widely called the "widow of the bump";
- Pain syndrome in the neck area, Nape.Discomfort improves by changing weather conditions, head movement;
- dance in blood pressure;
- extension and a more dangerous form of pathology with a rupture of a fibrous ring, bright pain syndrome - intervertebral disc hernia;
- severe headaches, including migraine -like nature;
- Numbers of the cervical region, shoulders, unpleasant tingling, pain and decreased wrist sensitivity.
To prevent cervical osteochondrosis, preventing the passage of pathology to a more severe degree 3, the patient should perform a doctor's prescription, take drugs, make gymnastics for the neck, participate in massage sessions, affect the problem area using a transdermal piece.It is important to abandon smoking, eat well, not kneeling, more often change your head position during your work day, but avoid sudden movements.Non -aging to be treated, irregularity of procedures, decreased chondroprotectors flow, frequent stress, hypothermia, hypodynamia are factors that increase the risk of cervical osteochondrosis.



















